Conservative management with medication and other non-surgical invasive therapies
Manejo conservador con medicación y otras terapias invasivas no quirúrgicas
Resumen:
La patología del manguito rotador es la causa más frecuente de dolor e incapacidad de hombro, con un porcentaje elevado de roturas irreparables. El tratamiento conservador es la primera opción en este tipo de roturas. Este incluye terapias físicas, mediación oral (antiinflamatorios no esteroideos –AINE–, tramadol) e infiltraciones con corticoides, ácido hialurónico y plasma rico en plaquetas, con resultados limitados a largo plazo. También puede optarse por un tratamiento invasivo con radiofrecuencia ablativa o pulsada, bien como primera opción o como alternativa al fracaso de los previamente citados.
Se recomienda la medicación oral con AINE o tramadol sobre todo para la mejora a corto plazo asociados con rehabilitación. Las infiltraciones con corticoides pueden proporcionar un alivio sintomático y una mejora funcional a corto plazo, pero con una alta variabilidad y sin diferencias respecto al tratamiento oral.
El ácido hialurónico se ha utilizado como alternativa condroprotectora a los corticoides, aunque son necesarios más estudios para sacar conclusiones relevantes, de la misma manera que el uso de plasma rico en plaquetas, que presenta una eficacia clínica incierta a corto plazo.
Por todo ello, las terapias invasivas, como la radiofrecuencia, han ganado interés. La neuroanatomía periférica del hombro permite identificar áreas potenciales de ablación, como el nervio supraescapular o axilar, pudiendo utilizar en ellas la radiofrecuencia ablativa o pulsada. Los resultados varían, pero algunos estudios sugieren alivio significativo del dolor y mejora funcional, pese a que se necesitan más estudios.
Se recomienda individualizar el tratamiento en cada caso, pudiendo combinar más de uno. Estos solo presentan mejoras a corto plazo, por lo que se necesitan nuevas alternativas para el manejo de estos pacientes a largo plazo y es ahí donde la neuromodulación emerge como una posible opción para el tratamiento conservador.
Abstract:
Rotator cuff disease is the most common cause of shoulder disability and pain, with a high percentage of irreparable ruptures. Conservative management is the first option in ruptures of this kind. This includes physical therapy, oral medication (nonsteroidal antiinflammatory drugs [NSAIDs], tramadol) and infiltrations of corticosteroid, hyaluronic acid and platelet rich plasma, with limited results over the long term. It is also possible to use ablative or pulsed radiofrequency, either as first choice or as an alternative after failure of the aforementioned treatments.
Oral medication with NSAIDs or tramadol is recommended especially for short term improvement, combined with rehabilitation. The infiltration of corticosteroids can provide symptoms relief with improved function over the short term, but with great variability and no differences versus oral treatment.
Hyaluronic acid has been used as a cartilage protecting alternative to corticosteroids, though further studies are needed in order to draw relevant conclusions, in the same way as with the use of platelet rich plasma, which shows uncertain clinical efficacy over the short term.
In view of the above, invasive therapies such as radiofrequency have gained interest. The peripheral neuroanatomy of the shoulder allows the identification of potential targets for ablation, such as the suprascapular or axillary nerve, using ablative or pulsed radiofrequency. The results vary, but some studies suggest significant pain relief and functional improvement - though further research is still needed.
It is advisable to individualize treatment in each case, with the possible combination of more than one option. Improvement is limited to the short term; new alternatives are thus needed for the management of these patients over the long term, and it is here where neuromodulation appears as a possible conservative management option.
Introduction
Rotator cuff disease is the most common cause of disability and the most prevalent condition seen in the clinical practice of shoulder surgeons(1). The overall incidence of rotator cuff rupture is between 5-40%(2), and among these injuries there are a significant number of massive ruptures (estimated at about 20%), as well as an important percentage of repeat ruptures (80%)(3). A distinction must be made between massive ruptures and irreparable ruptures, since the former are not necessarily irreparable. Massive ruptures are defined as ruptures presenting a size of > 5 cm in the coronal plane or which affect two or more tendons(4). The definition of irreparable rupture is more controversial. Although massive ruptures can be repaired, the failure rate is 25-94%, depending on the cases, over a follow-up period of two years, and is typically associated with biological failure of the tendon-bone junction(5). Thus, the identification and management of irreparable rotator cuff ruptures constitutes a challenge for surgeons in relation to cost-economical aspects and as regards the short and long term benefits for the patient(6).
Conservative management should be the first line option in ruptures of this kind, and may prove effective in some patients, despite progression of the size of the rupture, adipose infiltration and arthropathy(7). Conservative management includes physical therapy with muscle strengthening and re-education, supported by rehabilitation therapy, oral medication (nonsteroidal antiinflammatory drugs [NSAIDs]) and subacromial infiltrations of corticosteroids, hyaluronic acid (HA) and biological therapies (platelet rich plasma [PRP]). When initial conservative management fails, or in some cases where surgical options are contraindicated because of the age of the patient, failed previous surgeries or the impossibility of repairing the rotator cuff due to the characteristics of rupture, we have new alternatives that are increasingly investigated, such as ablative or pulsed radiofrequency (RF), which can also be useful as initial treatment in selected cases.
The present review addresses conservative management with medications, as well as infiltrations and invasive therapies for dealing with pain. It should be mentioned, however, that few studies have reviewed the results of these treatments(7), and most of them involve a combination of several such therapies, since no conservative management protocol has been established to date(8).
Prognostic factors in the conservative management of irreparable rotator cuff ruptures
Most studies define failed conservative management as the appearance or worsening of pain and/or loss of function, requiring surgical treatment. The overall success rate varies from 32-100%(9). Vad et al.(9) found the poorest outcomes to be associated with a decrease in strength in abduction and external rotation < 3/5, muscle atrophy, superior migration of the humeral head, reduction of the passive range of motion, and the evolution of glenohumeral arthropathy. Yian et al.(10) in turn found loss of flexion < 50° to be associated to poorer outcomes and failure of conservative management. Collin et al.(11) observed that failed conservative management was more common in anterior ruptures of the rotator cuff, though in contrast Agout et al.(12), found no correlation between the zone of rupture and treatment success. Yoon et al.(13) found that patients with an intact subscapularis or hypertrophy of the teres minor presented a 57% success rate with conservative management, versus 32% in patients without these characteristics.
Lastly, it is important to mention that conservative management appears to afford poorer outcomes in individuals with chronic symptoms, defined as those with a duration of over 6 months, in reference to both pain and loss of function(14).
Oral medication
As has been mentioned, oral medication should be the first line of treatment, particularly in patients with low functional demands and comorbidities that contraindicate other types of treatment, and in individuals who develop symptoms or worsen following contusion or trauma, without their limitations having an impact upon the basic activities of daily living(15). According to a systematic review of the clinical practice guides(16), it is possible to recommend both NSAIDs and tramadol hydrochloride to treat pain and improve function, as well as hypnotics for the sleep disturbances which some patients may experience.
These treatments, combined with physical and rehabilitation therapy, can help alleviate pain and improve function, but the results persist only over the short term(17).
Corticosteroids
The use of corticosteroid infiltrations in shoulder disease is a very widespread practice. There is agreement that corticosteroids suppress acute inflammation through inhibition of the protein synthesis of proinflammatory products. Likewise, they afford symptoms relief and transient functional improvement in both rotator cuff disease and in other conditions characterized by shoulder pain (adhesive capsulitis, primary arthropathy,etc.)(18), despite their side effects(19) and the negative impact they appear to have upon the tendon(20). According to the American Academy of Orthopedic Surgeons (AAOS), a single injection along with local anesthetic affords short term symptoms relief and improved joint function(21). A systematic Cochrane review(22) on corticosteroid infiltrations concluded that in the case of rotator cuff disease, the literature offers heterogeneous results referred to benefit compared with the use of placebo at four weeks, with benefit ranging from minor to no significant differences (the studies moreover being variable in terms of methodological quality). Likewise, no significant differences were observed on comparing corticosteroids versus oral NSAIDs. Thus, based on these results, it is difficult to draw any conclusions regarding the short and long term benefits of subacromial corticosteroid infiltrations.
Hyaluronic acid
Due to the potential negative effects of the above treatments, in the last two decades HA infiltration has emerged as an alternative for the conservative management of arthropathy(23), though few articles have investigated its effects in application to rotator cuff injuries. Hyaluronic acid has both analgesic and cartilage protecting properties(23). A review(24) including 11 articles related to HA infiltration in rotator cuff disease and involving a total of 1102 patients concluded that such infiltration improves symptoms and function in patients with rotator cuff lesions, with no adverse effects or reactions. It thus may constitute an alternative to the previous therapies, in view of its biochemical and biomechanical properties - though further studies are needed to determine the most effective molecular weight, and define when and in what lesion grades it should be administered.
Another systematic review and meta-analysis(25) related to the conservative management of arthropathy, including 15 and 7 studies, respectively, documented a significant decrease in pain after three and 6 months of follow-up, as well as functional improvement at all the follow-up timepoints. The comparative studies yielded similar results regarding pain relief versus placebo, saline solution or corticosteroids, and a strong placebo effect was observed in intraarticular injection in the shoulder. Here again there is a need for greater quality randomized clinical trials to assess efficacy, optimum dose, molecular weight and administration routes. As a result, no recommendation referred to the use of HA can be established at this time.
Platelet rich plasma
In a way similar to the treatment described above, there has recently been an increased in the interest and use of PRP injections for the conservative management of rotator cuff disease(26). Platelet rich plasma is an autologous blood product containing abundant growth factors and bioactive cytokines that reduce inflammation and facilitate healing, incrementing cell migration and proliferation, and favoring angiogenesis(27,28). However, there is considerable debate regarding its clinical efficacy, and consensus is lacking as to the usefulness of PRP in rotator cuff disease(29). A systematic review of randomized clinical trials on the use of PRP in rotator cuff disease(30) involving control groups suggests that over the short term, PRP might not be of benefit compared with the control therapies (physical exercise, placebo, corticosteroids), in terms of either improved pain perception or functional improvement. Despite this, the use of PRP is growing, and the existing scientific evidence is still inconsistent. Further studies of greater quality are needed, standardizing the type of rupture and its size, the preparation of PRP and the injected dosage.
Invasive therapies. Nerve blocks and radiofrequency
Due to the high prevalence and potential persistence of shoulder pain, the continued development of new treatments for pain in this region is crucial(31). Nerve ablation is an established strategy for the middle to long term alleviation of persistent pain in other joints(32). Considering that there is a large proportion of patients with chronic and refractory shoulder pain, and that many of them are not candidates for surgery, the existence of shoulder neuroablation protocols is considered necessary(33). We therefore need to know the sensory innervation of the shoulder.
Peripheral neuroanatomy of the shoulder
Suprascapular nerve
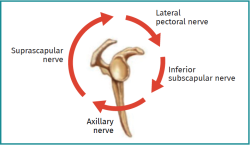
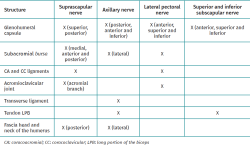
The suprascapular nerve arises from the superior trunk of the brachial plexus. It gives rise to three main articular branches (non-motor): the medial subacromial branch, the lateral subacromial branch and the posterior glenohumeral branch(34). The first branch innervates the coracoclavicular and acromioclavicular ligaments, and the medial portion of the subacromial bursa; the second branch innervates the lateral portion of the subacromial bursa and the acromioclavicular ligaments; and the third branch innervates the posterior capsule of the glenohumeral joint(31) (Figure 1).
Axillary nerve
The axillary nerve originates in the posterior fascicle of the brachial plexus. Over its trajectory, the nerve divides into an anterior branch and a posterior branch. On crossing the quadrangular space, the anterior division (which innervates the middle and anterior portion of the deltoid muscle) emits deep articular branches to the tendon of the subscapularis, innervating the anteroinferior capsule(35). Additional branches surround the humerus from posterior to anterolateral, innervating the transverse ligament of the humerus and the tendon of the long head of the biceps. In 60% of the studied specimens, branches from the anterior division run superiorly and in depth to the deltoid muscle to innervate the lateral portion of the subacromial bursa. The posterior division in turn innervates the teres minor and the posterior region of the deltoid muscle, and emits articular branches to the inferior glenohumeral ligament and the posteroinferior capsule(36) (Figure 1).
Lateral pectoral nerve
This nerve arises from the lateral fascicle of the brachial plexus and innervates the greater pectoral muscle (pectoralis major). A sensory portion crosses medial to lateral superficial to the coracoid process. It has been seen that this articular branch crosses more consistently at the midpoint between the tip of the coracoid process and the clavicle. It emerges anterior to the acromioclavicular joint, in the coracoacromial and coracoclavicular ligaments, in the subacromial bursa and in the anterior glenohumeral capsule(37) (Figure 1).
Superior and inferior subscapular nerves
These nerves originate in the posterior fascicle of the brachial plexus, or sometimes from the axillary nerve, respectively. They provide motor innervation for the subscapularis muscle, followed by the emission of submuscular articular branches(38). The superior subscapular nerve innervates the anterosuperior capsule, while the inferior nerve innervates the tendon of the long head of the biceps(39) (Figure 1).
Ablation zones for the treatment of shoulder pain(31)
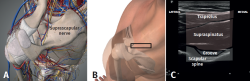
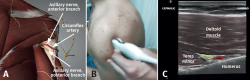
Based on detailed reviews of the zones available for ablation and with current knowledge of the innervation of the shoulder, four potential ablation zones are recommended. However, despite the current use of the technique, further studies and validation are needed. On performing ablation lateral to the supraglenoid groove, at the upper half of the glenoid neck in its posterosuperior region, the subacromial lateral and posterior glenohumeral branches of the suprascapular nerve may be affected, without damaging its motor component (Figure 2). In order to target the subacromial medial branch of the suprascapular nerve, the location must be in the anterosuperior portion of the glenoid neck, near the base of the coracoid process. The ascending branches of the axillary nerve are usually found close to the junction between the posteroinferior margin of the greater tubercle and the metaphysis of the humerus (Figure 3). According to the above description referred to the trajectory of the articular branch of the lateral pectoral nerve, its safe ablation would be in the superficial middle zone of the coracoid process. Motor stimulation must be performed in all these zones in order to avoid damaging the motor fibers. Thus, on performing nerve ablation of the shoulder, we would be carrying out denervation mainly of the following targets: anterosuperior and middle-posterosuperior glenohumeral capsule, subacromial bursa, the coracoacromial and coracoclavicular ligaments, and the acromioclavicular joint (Table 1).
Types of radiofrequency: ablative and pulsed
Ablative radiofrequency is performed at temperatures of 70-80ºC, and results in neuron destruction(40). In application to sensorimotor nerves, ablative radiofrequency may affect motor function. For this reason pulsed radiofrequency began to be used as an alternative, since it involves temperatures of between 40-45ºC, thus avoiding the loss of neuron function but exerting a neuromodulatory effect that contributes to analgesia(41). The procedure usually involves the induction of a prognostic anesthetic block, and if the pain is seen to decrease by over 50%, the corresponding technique is applied. The most commonly used pulsed radiofrequency sequence consists of pulses of 2 Hz spaced 20 ms apart, and with a duration of 2-10 minutes(41).
Results of radiofrequency
Despite the above observations, there is a lack of due evaluation of the results obtained with the two types of radiofrequency treatment in application to the innervation of the shoulder joint. Furthermore, there is considerable variability of the neural targets in radiofrequency procedures.
A systematic review and meta-analysis(42) analyzed the results of these procedures in terms of function, pain improvement and adverse effects, as outcomes of interest. The primary result was the change in pain intensity while the secondary results were referred to function, mobility, strength, disability and patient quality of life or satisfaction. A total of 42 studies were reviewed (36 related to pulsed radiofrequency and 6 to ablative radiofrequency). The origin of the pain included rotator cuff disease and adhesive capsulitis as the two most common diagnoses. Most of the studies were focused on the application of radiofrequency over the suprascapular nerve, with secondary emphasis on the rest of the nerves. On performing a meta-analysis of 7 randomized clinical trials comparing pulsed radiofrequency versus a control group, the evidence was found to be poor, with doubtful results indicating that pulsed radiofrequency affords analgesia and functional improvement versus conventional medical treatment of chronic shoulder pain.
In relation to the review of case series, most of the publications reported a more than 50% decrease in pain with pulsed radiofrequency, with a duration of effect of between days and up to two years. In the case of ablative radiofrequency, all the studies reported a pain intensity reduction of over 50%. The case series on ablative and pulsed radiofrequency also evidenced improvements in function in most studies. There were no important adverse effects. This study highlights the need for new studies focused on other ablation therapeutic targets, scale-based registries, clinical studies evaluating different imaging techniques for performing radiofrequency, and comparative studies of the different ablation techniques.
Conclusions
Many conservative management options are available for irreparable rotator cuff ruptures, though none have been shown to be superior to the rest. It is therefore advisable to individualize each case, with the possibility of combining more than one treatment option. Most of these treatments have only shown improvements over the short term. We therefore need to continue searching for therapies that can reduce pain and improve function over the middle and long term - and this is where radiofrequency and the different pain neuromodulation strategies may find an application. Nevertheless, studies of greater methodological quality are needed.
Figuras
Figure 2. A: anatomy of the suprascapular nerve; B: view of ultrasound probe placement for locating the suprascapular nerve; C: ultrasound view of the supraglenoid groove.
Figure 3. A: anatomy of the axillary nerve; B: view of ultrasound probe placement for locating the axillary nerve; C: ultrasound view of the axillary nerve and arteries.
Tablas
Información del artículo
Cita bibliográfica
Autores
Carlos Vaquero Comino
Traumatología y Cirugía Ortopédica. Hospital ASEPEYO. Coslada, Madrid
Miguel García Navlet
Grupo +QTrauma. Hospital Beata María Ana. Madrid
Sección de Traumatología, Unidad de patología de hombro y codo, Hospital ASEPEYO, Coslada, Madrid, España
Unidad de Hombro y Codo. +QTrauma. Hospital Beata María Ana. Madrid
Arancha Hernando Sánchez
Traumatología y Cirugía Ortopédica. Hospital ASEPEYO. Coslada, Madrid
Alejandro Ortega Romero
Servicio de Anestesiología y Tratamiento del Dolor. Hospital Monográfico de Traumatología y Rehabilitación ASEPEYO. Coslada. Madrid
Domingo Manzano Gaspar
Servicio de Anestesiología y Tratamiento del Dolor. Hospital Monográfico de Traumatología y Rehabilitación ASEPEYO. Coslada. Madrid
Ethical responsibilities
Conflicts of interest. The authors state that they have no conflicts of interest.
Financial support. This study has received no financial support.
Protection of people and animals. The authors declare that this research has not involved human or animal experimentation.
Data confidentiality. The authors declare that the protocols of their work centre referred to the publication of patient information have been followed.
Right to privacy and informed consent. The authors declare that no patient data appear in this article.
Referencias bibliográficas
-
1Yamaguchi K, Ditsios K, Middleton WD, et al. The demographic and morphological features of rotator cuff disease. A comparison of asymptomatic and symptomatic shoulders. J Bone Joint Surg Am. 2006;88:1699-704.
-
2Kovacevic D, Suriani RJ Jr, Grawe BM, et al. Management of irreparable massive rotator cuff tears: a systematic review and meta-analysis of patient-reported outcomes, reoperation rates, and treatment response. J Shoulder Elbow Surg. 2020 Dec;29(12):2459-75.
-
3Lo IK, Burkhart SS. Arthroscopic revision of failed rotator cuff repairs: technique and results. Arthroscopy. 2004;20:250-67.
-
4Gerber C, Fuchs B, Hodler J. The results of repair of massive tears of the rotator cuff. J Bone Joint Surg Am. 2000;82:505-15.
-
5Kim SJ, Kim SH, Lee SK, Seo JW, Chun YM. Arthroscopic repair of massive contracted rotator cuff tears: Aggressive release with anterior and posterior interval slides do not improve cuff healing and integrity. J Bone Joint Surg Am. 2013;95:1482-8.
-
6Cvetanovich GL, Waterman BR, Verma NN, Romeo AA. Management of the Irreparable Rotator Cuff Tear. J Am Acad Orthop Surg. 2019 Dec 15;27(24):909-17.
-
7Zingg PO, Jost B, Sukthankar A, Buhler M, Pfirrmann CWA, Gerber C. Clinical and structural outcomes of nonoperative management of massive rotator cuff tears. J Bone Joint Surg Am. 2007;89:1928-34.
-
8Shepet KH, Liechti DJ, Kuhn JE. Nonoperative treatment of chronic, massive irreparable rotator cuff tears: a systematic review with synthesis of a standardized rehabilitation protocol. J Shoulder Elbow Surg. 2021 Jun;30(6):1431-44.
-
9Vad VB, Warren RF, Altchek DW, O’Brien SJ, Rose HA, Wickiewicz TL. Negative prognostic factors in managing massive rotator cuff tears. Clin J Sport Med. 2002;12(3):151-7.
-
10Yian EH, Sodl JF, Dionysian E, Schneeberger AG. Anterior deltoid reeducation for irreparable rotator cuff tears revisited. J Shoulder Elbow Surg. 2017;26(9):1562-5.
-
11Collin PG, Gain S, Nguyen Huu F, Lädermann A. Is rehabilitation effective in massive rotator cuff tears? Orthop Traumatol Surg Res. 2015;101(4 Suppl):S203-5.
-
12Agout C, Berhouet J, Spiry C, Bonnevialle N, Joudet T, Favard L. Functional outcomes after non-operative treatment of irreparable massive rotator cuff tears: Prospective multicenter study in 68 patients. Orthop Traumatol Surg Res. 2018;104(8S):S189-S192.
-
13Yoon TH, Kim SJ, Choi CH, Yoon SP, Chun YM. An intact subscapularis tendon and compensatory teres minor hypertrophy yield lower failure rates for non-operative treatment of irreparable, massive rotator cuff tears. Knee Surg Sports Traumatol Arthrosc. 2019;27(10):3240-5.
-
14Bokor DJ, Hawkins RJ, Huckell GH, Angelo RL, Schickendantz MS. Results of nonoperative management of full-thickness tears of the rotator cuff. Clin Orthop Relat Res. 1993:103-10.
-
15Oh JH, Park MS, Rhee SM. Treatment Strategy for Irreparable Rotator Cuff Tears. Clin Orthop Surg. 2018 Jun;10(2):119-34.
-
16Doiron-Cadrin P, Lafrance S, Saulnier M, et al. Shoulder Rotator Cuff Disorders: A Systematic Review of Clinical Practice Guidelines and Semantic Analyses of Recommendations. Arch Phys Med Rehabil. 2020 Jul;101(7):1233-42.
-
17Juhan T, Stone M, Jalali O, et al. Irreparable rotator cuff tears: Current treatment options. Orthop Rev (Pavia). 2019 Sep 30;11(3):8146.
-
18Adra M, El Ghazal N, Nakanishi H, et al. Platelet-rich plasma versus corticosteroid injections in the management of patients with rotator cuff disease: a systematic review and meta-analysis. J Orthop Res. 2023 Jan;41(1):7-20.
-
19Shibata Y, Midorikawa K, Emoto G, Naito M. Clinical evaluation of sodium hyaluronate for the treatment of patients with rotator cuff tear. J Shoulder Elbow Surg. 2001 May-Jun;10(3):209-16.
-
20Ford LT, DeBender J. Tendon rupture after local steroid injection. South Med J. 1979;72:827-30.
-
21Weber S, Chahal J. Management of rotator cuff injuries. J Am Acad Orthop Surg. 2020;28:e193-e201.
-
22Buchbinder R, Green S, Youd JM. Corticosteroid injections for shoulder pain. Cochrane Database Syst Rev. 2003;2003(1):CD004016.
-
23Brockmeier SF, Shaffer BS. Viscosupplementation therapy for osteoarthritis. Sports Med Arthrosc. 2006;14:155-62.
-
24Osti L, Buda M, Buono AD, Osti R, Massari L. Clinical evidence in the treatment of rotator cuff tears with hyaluronic acid. Muscles Ligaments Tendons J. 2016 Feb 13;5(4):270-5.
-
25Zhang B, Thayaparan A, Horner N, Bedi A, Alolabi B, Khan M. Outcomes of hyaluronic acid injections for glenohumeral osteoarthritis: a systematic review and meta-analysis. J Shoulder Elbow Surg. 2019 Mar;28(3):596-606.
-
26Zhang JY, Fabricant PD, Ishmael CR, Wang JC, Petrigliano FA, Jones KJ. Utilization of Platelet-Rich Plasma for Musculoskeletal Injuries: An Analysis of Current Treatment Trends in the United States. Orthop J Sports Med. 2016 Dec 21;4(12):2325967116676241.
-
27Baksh N, Hannon CP, Murawski CD, Smyth NA, Kennedy JG. Platelet-rich plasma in tendon models: A systematic review of basic science literature. Arthroscopy. 2013;29:596-607.
-
28Boswell SG, Cole BJ, Sundman EA, Karas V, Fortier LA. Platelet-rich plasma: A milieu of bioactive factors. Arthroscopy. 2012;28:429-39.
-
29Hurley ET, Hannon CP, Pauzenberger L, Fat DL, Moran CJ, Mullett H. Nonoperative Treatment of Rotator Cuff Disease With Platelet-Rich Plasma: A Systematic Review of Randomized Controlled Trials. Arthroscopy. 2019 May;35(5):1584-91.
-
30Surace SJ, Deitch J, Johnston RV, Buchbinder R. Shock wave therapy for rotator cuff disease with or without calcification. Cochrane Database Syst Rev. 2020 Mar 4;3(3):CD008962.
-
31Eckmann MS, McCormick ZL, Beal C, Julia J, Cheney CW, Nagpal AS. Putting Our Shoulder to the Wheel: Current Understanding and Gaps in Nerve Ablation for Chronic Shoulder Pain. Pain Med. 2021 Jul 25;22(Suppl 1):S2-S8.
-
32Dellon AL. Shoulder denervation. In: Joint Denervation: Anatomic Atlas of Surgical Techniques. Switzerland: Springer Nature; 2019:107-32.
-
33Eckmann MS, Bickelhaupt B, Fehl J, et al. Cadaveric Study of the Articular Branches of the Shoulder Joint. Reg Anesth Pain Med. 2017 Sep/Oct;42(5):564-70.
-
34Laumonerie P, Blasco L, Tibbo ME, et al. Sensory innervation of the subacromial bursa by the distal suprascapularnerve: a new description of its anatomic distribution. J Shoulder Elbow Surg. 2019;28:1788-94.
-
35Nasu H, Nimura A, Yamaguchi K, Akita K. Distribution of the axillary nerve to the subacromial bursa and the area around the long head of the biceps tendon. Knee Surg Sports Traumatol Arthrosc. 2015;23:2651-7.
-
36Bickelhaupt B, Eckmann MS, Brennick C, Rahimi OB. Quantitative analysis of the distal, lateral, and posterior articular branches of the axillary nerve to the shoulder: Implications for intervention. Reg Anesth Pain Med. 2019;44(9):875-80.
-
37Nam YS, Panchal K, Kim IB, Ji JH, Park MG, Park SR. Anatomical study of the articular branch of the lateral pectoral nerve to the shoulder joint. Knee Surg Sports Traumatol Arthrosc. 2016;24:3820-7.
-
38Tran J, Peng PWH, Agur AMR. Anatomical study of the innerva- tion of glenohumeral and acromioclavicular jointcapsules: Implications for image-guided intervention. Reg Anesth Pain Med. 2019;44(4):452-8.
-
39Laumonerie P, Dalmas Y, Tibbo ME, et al. Sensory innervation of the human shoulder joint: The three bridges to break. J Shoulder Elbow Surg. 2020;29(12):e499-e507.
-
40Bone ME, Armstrong A, Bashir I, Haynes J. Thermal radiofrequency denervation of the suprascapular nerve for chronic shoulder pain. Shoulder Elbow. 2013;5(4):226-30.
-
41Chua NHL, Vissers KC, Sluijter ME. Pulsed radiofrequency treatment in interventional pain management: Mechanisms and potential indications—A review. Acta Neurochirurgica. 2011;153(4):763-71.
-
42Pushparaj H, Hoydonckx Y, Mittal N, et al. A systematic review and meta-analysis of radiofrequency procedures on innervation to the shoulder joint for relieving chronic pain. Eur J Pain. 2021 May;25(5):986-1011.
Descargar artículo:
Licencia:
Este contenido es de acceso abierto (Open-Access) y se ha distribuido bajo los términos de la licencia Creative Commons CC BY-NC-ND (Reconocimiento-NoComercial-SinObraDerivada 4.0 Internacional) que permite usar, distribuir y reproducir en cualquier medio siempre que se citen a los autores y no se utilice para fines comerciales ni para hacer obras derivadas.
Comparte este contenido
En esta edición
- Sometimes the rotator cuff injury of the shoulder is not repairable and we will have to do something with it…
- More manuscripts!
- Teach everything, tell everything
- Irreparable massive ruptures of the posterosuperior cuff: definition, diagnosis and classification
- Conservative management with medication and other non-surgical invasive therapies
- Physiotherapy and electrophysical therapies in the conservative management of irreparable posterosuperior rotator cuff rupture
- Alternatives in irreparable ruptures of the posterosuperior cuff. Debridement, tenotomy, partial repair
- Surgical alternatives in irreparable ruptures of the posterosuperior cuff
- Tendon transfers in irreparable ruptures of the posterosuperior rotator cuff. Latissimus dorsi and lower trapezius
- Reverse replacement in a patient without osteoarthritis
- Arthroscopic surgical technique for tendon transfer of the lower trapezius
- Arthroscopy assisted latissimus dorsi transfer for irreparable posterosuperior rotator cuff injuries really works
- Instructions for authors (Sept. 2023)
Más en PUBMED
Más en Google Scholar


Revista Española de Artroscopia y Cirugía Articular está distribuida bajo una licencia de Creative Commons Reconocimiento-NoComercial-SinObraDerivada 4.0 Internacional.